Accomplished CTV News reporter, John Vennavally-Rao was feeling fine at age 53. He was hitting the gym regularly, running a few times a week, and generally taking care of himself. He had no symptoms. No warning signs. Nothing that would make him think twice about scheduling a routine colonoscopy.
Then came the diagnosis of two separate, advanced cancers — one in his rectum and one in his lung.
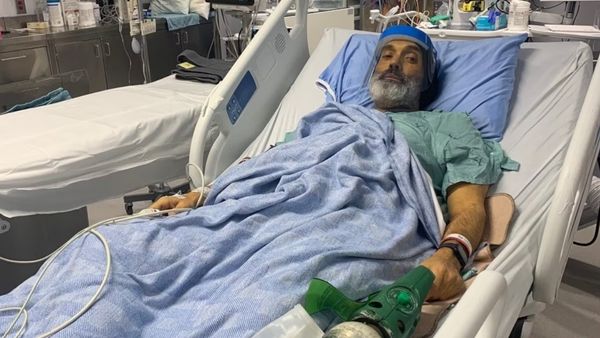
“I thought I just dodged a bullet,” John recalls. “Turns out, I was standing right in the crosshairs.”
His story isn’t uncommon. It’s a reminder that colorectal cancer doesn’t care how healthy you feel, how much you exercise, or how many vegetables you eat. And increasingly, it’s not just a disease of older men.
Why screening matters more than you think
Dr. Brian Bressler, a gastroenterologist, puts it plainly. “The only thing that’s been proven to reduce your risk of colorectal cancer is regular screening.”
That’s right. Screening itself is a lifestyle measure. It’s proactive health care that catches problems before they become emergencies. For decades, the standard screening age in Canada has been 50, but that criterion is shifting.
“We’re seeing colon cancer being diagnosed more frequently in patients under 50,” Dr. Bressler notes. “It’s happening in an alarming way.” Emerging research highlights this and diagnoses are expected to double. As scary as that seems, colorectal cancer (when caught early) has a survival rate of 90% — that’s huge. It means the earlier we catch these cases, the more likely it is for men to recover.
In the U.S. the recommended screening age has already dropped to 45. Recently, the Canadian Cancer Society has voiced its concern about colorectal screening ages to reach the same benchmark as our southern neighbours.
Know your body, know your risks
The thing about colorectal cancer is that it often doesn’t show symptoms until it’s advanced. That’s why screening is so critical. But if you do notice changes, don’t ignore them.
Red flags to watch for:
- Blood in your stool (this is not normal)
- A change in your bowel movement routine that persists
- Abdominal discomfort that won’t go away
- Iron deficiency anemia without an obvious cause
Dr. Bressler emphasizes that “normal” bowel habits vary from person to person. What really matters is whether your routine has changed. If you’ve noticed something different that lasts more than a couple of weeks, talk to your doctor.
And don’t let embarrassment get in the way. “It’s not really acceptable in society to talk about bowels,” Dr. Bressler admits. “That’s unfortunate.”
John shares a similar thought. He’s heard stories of men bleeding for six months before seeking help because they were too embarrassed to bring it up. “You gotta get that stuff checked out,” he says.
Younger men, higher risk

One of the most concerning trends in colorectal cancer is the rise in early-onset cases. While we’re still discovering why, experts point to potential factors like inactive lifestyles, poor eating habits and environmental influences.
“If you’re 43 years old and you have a change in bowel habit and some blood in your stool, don’t assume it’s not cancer because you’re under 50,” Dr. Bressler warns. “It’s probably not cancer, but we have a much lower threshold to investigate those symptoms in younger patients than we have had in the past.”
Family history also matters. If you have a close relative who was diagnosed with colorectal cancer before 60, your screening should likely start earlier.
What you can control
While screening is the only proven prevention method, lifestyle choices still matter. Research suggests associations between colorectal cancer and things like obesity, ultra-processed foods and alcohol intake.
And although it’s never a total guarantee, maintaining a healthy weight, eating a balanced diet and staying active are always smart moves when it comes to disease prevention.
John’s fitness routine, for example, likely played a role in his recovery. “Having that extra muscle mass really helped get me through that surgery,” he says. During a month-long hospital stay, he lost 30 pounds, mostly muscle.
“It’s amazing,” he says. “You go from jogging 30 minutes a day to barely being able to walk in the course of three weeks in hospital. The speed at which you can deteriorate is breathtaking.”
Thankfully because he’d built up reserves over years of weightlifting, he had the strength to pull himself up in bed and eventually get back to the gym.
How to catch it early

Screening options in Canada typically include:
- Fecal immunochemical test (FIT): A stool-based kit mailed to your home. Easy to do but less accurate than a colonoscopy.
- Colonoscopy: The gold standard. More invasive but more thorough.
If you’re at an increased risk for colorectal cancer, some experts recommend a colonoscopy over a FIT test.
John doesn’t dance around the bush when it comes to screening options. “Get screened. Advocate for yourself. Maybe get a second opinion. The person that’s going to look out for you the most is yourself.”
He’s learned to read his own lab reports, catch mistakes and have more informed conversations with his doctors. “It’s empowering,” he says. “But if that’s stressful for you, maybe it’s better to let somebody else be in the driver’s seat.”
Hope on the horizon
Despite everything John’s been through, he’s optimistic. Medical advances have given him a fighting chance that previous generations didn’t have. His lung cancer has a specific gene mutation that can be targeted with medication. His surgeries were minimally invasive. His recovery, while difficult, has been possible.
“I’m super grateful that they were able to do any of this,” he says. “Twenty years ago, somebody like me would have probably lived about a year and a half. Just so much progress has been made.”
He’s also grateful for the awareness his story has created. Since sharing his experience, he’s received messages from people across Canada — some with similar diagnoses, others with questions about ostomy bags, others just wanting to know they’re not alone.
Take action today
You don’t have to wait for symptoms. You don’t have to wait until you’re 50. And you definitely don’t have to face this alone.
Talk to your primary care doctor about when to start screening. If you notice changes in your body, speak up. And remember, taking action early is always better than waiting until it’s too late.
ARE YOU AT RISK?
Learn your risk level for the most common men’s health conditions in 10 minutes with a free, confidential, and personalized report.







‘this is scary. I’m 78 with colonoscopies every 5 years. Should I feel safe or get checked annually?
Sounds like you’re already on top of your regular check ups, so don’t stress too much! It’s great that you’re being proactive about your health. Your doctor is still the best person for advice when it comes to your health.
~Canadian Men’s Health Foundation Team